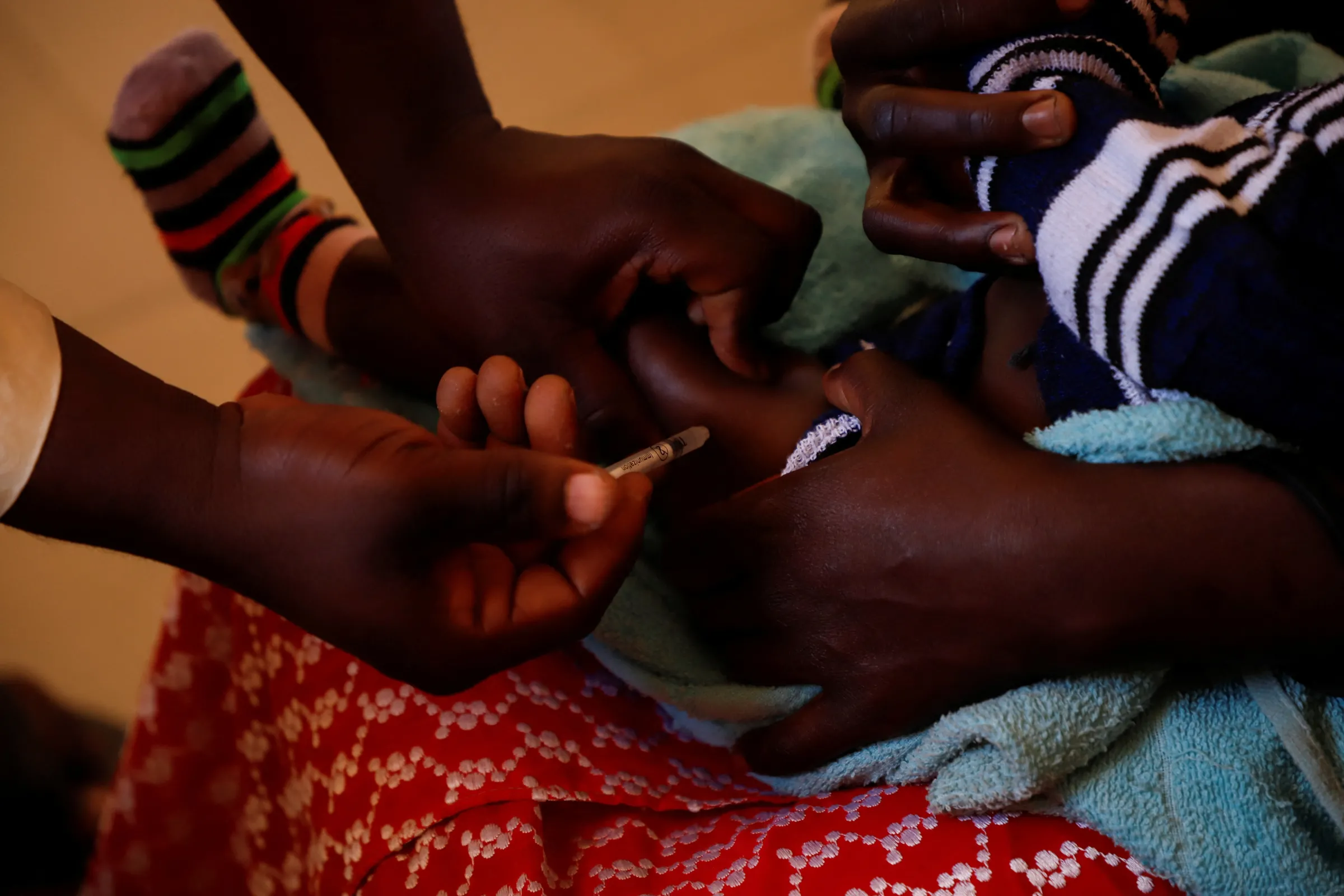
From Ukraine to Gaza: Can health systems adapt and thrive in times of crisis?
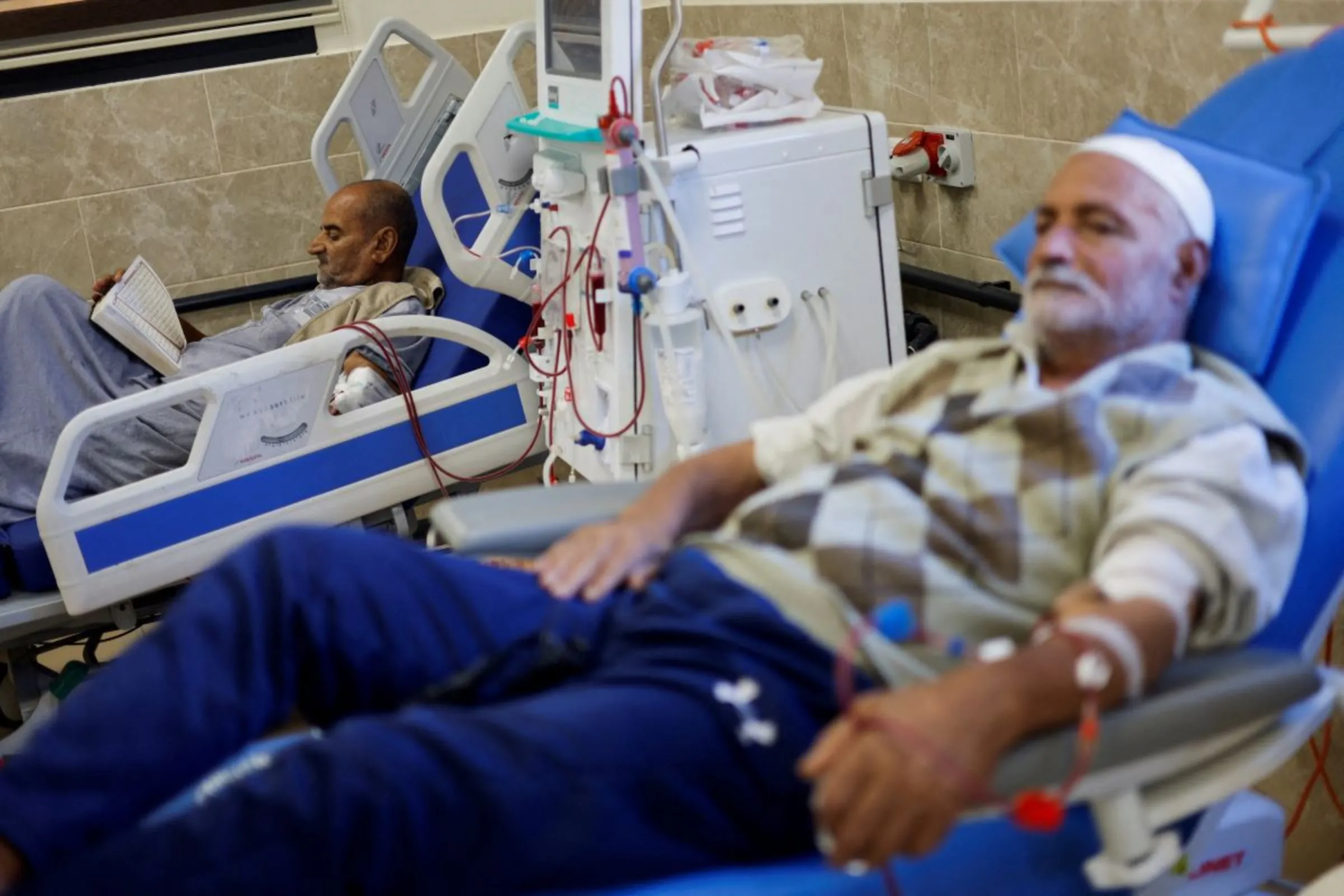
A Palestinian kidney patient reads while lying on a hospital bed, as health officials say they are running out of fuel to operate dialysis devices, amid the ongoing Israeli-Palestinian conflict, at Naser hospital in Khan Younis in the southern Gaza Strip October 15, 2023. REUTERS/Mohammed Salem
Latest crises in Gaza, Libya and Ukraine highlight the pressures of war, climate change and economic downturn on health systems
Jorge Moreira Da Silva is UN Under-Secretary-General and Executive Director of UNOPS (UN’s infrastructure and procurement specialists). UNOPS hosted a high-level panel discussion at the World Health Summit on 16 October, titled “Fostering Health System Resilience in Fragile and Conflict-Affected Countries”.
2023 has been called “a defining year for global health action”. This week, leaders, scientists, businesses and civil society organizations from around the world gathered in Berlin to set the agenda for a healthier future.
A focus on actions cannot come soon enough, in a world where the vulnerabilities of health systems continue to be laid bare by climate change, conflicts, the continued evolution of COVID-19, and ongoing cost of living and debt crises. For those most vulnerable, these ongoing crises can create a ‘perfect storm’ that obliterates years of progress in health.
Over the past few days, the humanitarian crisis in Gaza has tragically demonstrated the extent of the pressures that conflicts exert on health systems. Attacks on health services, lack of power, water and supplies simply mean that hospitals cannot save lives.
Last month’s floods in Libya painted another tragic picture: Thousands lost their lives, many more were displaced, and communities were left without access to basic and health services. Years of conflict and political instability have degraded critical infrastructure and weakened health systems, while the impact of climate change made the storms more likely and intense.
Nearly a quarter of the global population currently live in settings affected by conflict, displacement and natural disasters. Of the 25 countries most vulnerable to climate change and least ready to adapt, the majority are also experiencing armed conflict. And the health consequences of climate change are costly: with direct damage to health estimated to cost between US$ 2–4 billion per year by 2030.
Conflict has a far-reaching impact on the health of individuals and communities ―from direct injury and violence, to displacement and mental and psychological trauma. Conflict also disrupts healthcare systems, damages critical infrastructure, impedes the supply of essential medicines, and hinders access to clean water and sanitation facilities. And the climate crisis is compounding existing fragilities.
Building resilient health systems is key, if we are to deliver on the promise of leaving no one behind.
How can we design, build and maintain health facilities that can cope with climate-related shocks?
How can we ensure that health facilities have access to clean and reliable energy?
How can we make sure they have the supplies that they need to run?
How do we make sure they are well-staffed? And that those healthcare workers are adequately trained and paid?
This ―and many others― are among the issues that my colleagues at UNOPS frequently encounter. At UNOPS, we take on sustainable development operations on behalf of our partners, including other UN agencies, donors and governments, through our expertise in infrastructure, procurement and project management.
We work closely with UN agencies mandated in health and humanitarian action, and we implement health projects and programmes in some of the most difficult operating environments around the world. In fact, health projects constitute our largest sector, and a third of our total delivery since 2016. There are many lessons that we have learnt about practical solutions that can improve access to health even amid active conflict.
Take Yemen, for example, where years of conflict have severely undermined the health system, leaving 20.3 million people without access to critical health services. Here, with support from Germany, we have been working to improve access to healthcare by rehabilitating and equipping key public health services. This work, which benefits around 3.4 million people, includes renovating facilities and hospital wards to upgrade water infrastructure and increase energy efficiency, while incorporating important gender considerations.
Yet so much more is needed: Around half of Yemen’s health facilities are still partially functional or not working because of lack of staff, funding and power shortages, as well as lack of medicines, supplies and equipment.
In Ukraine, amid ongoing conflict, my colleagues are working with partners to improve the effectiveness of medical services by providing reliable energy sources as well as procuring and delivering essential medical equipment. Here, too, the challenge is maintaining a long-term focus on building stronger health systems, while responding to immediate needs.
There is no development without health. The most vulnerable populations in fragile and conflict-affected areas need urgent action and investment to improve access to healthcare. Action that responds to today’s needs, while building the foundation for a resilient, inclusive and sustainable future.
Any views expressed in this opinion piece are those of the author and not of Context or the Thomson Reuters Foundation.
Tags
- Finance
- Government aid
- Wealth inequality
- War and conflict
Go Deeper
Related
MORE ON Rethinking the Economy
Latest on Context
- 1
- 2
- 3
- 4
- 5
- 6