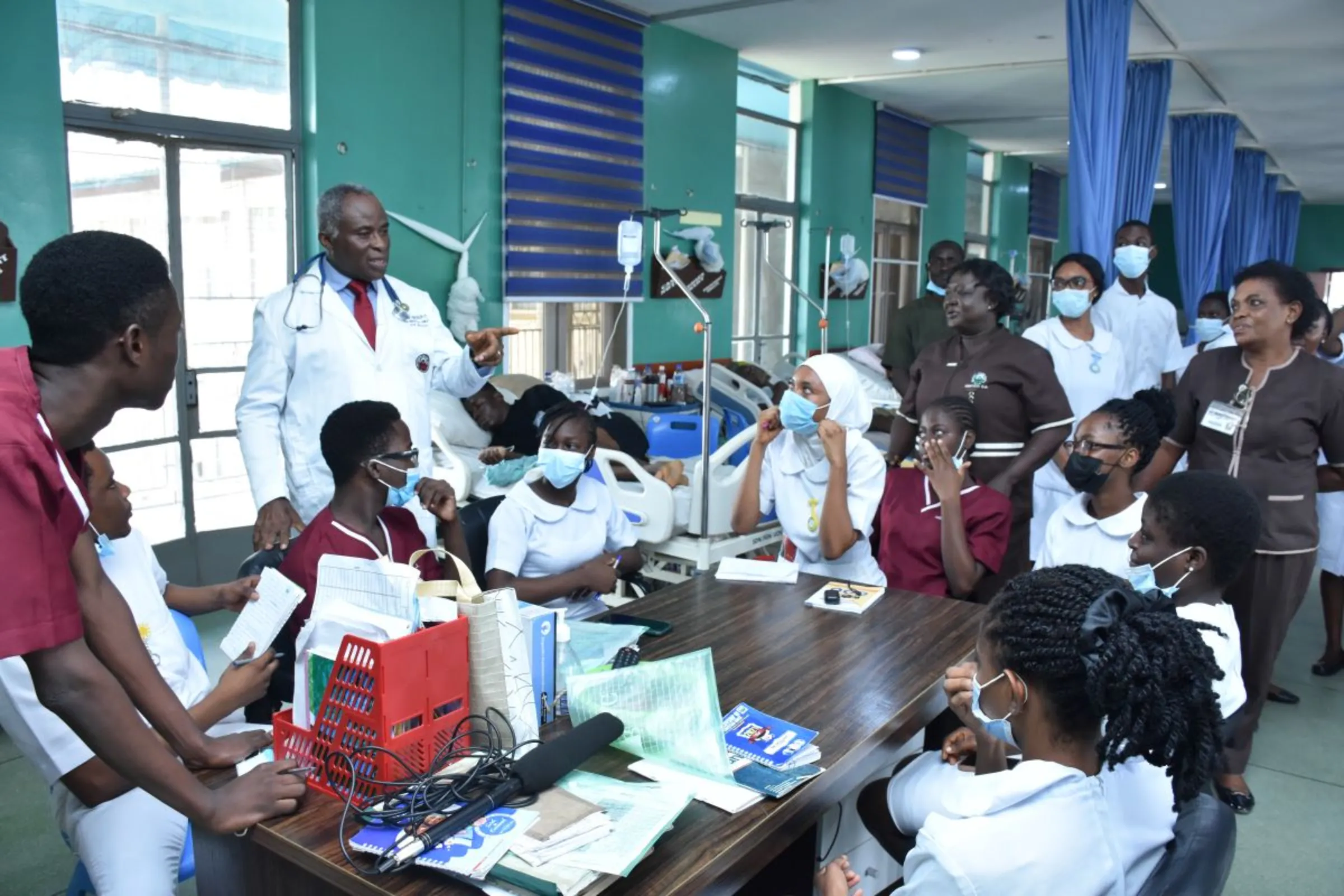
African hospitals suffer as nurses leave for more pay in UK

Nurses during a ward round at the University Teaching College Hospital, Ibadan in Nigeria on May 8, 2023. Bukola Adebayo/Thomson Reuters Foundation.
What’s the context?
Poor pay drives Nigerian and Zimbabwean nurses to work in UK, leaving their own health systems on the brink
- Shortage of nurses means wards closing, hospitals say
- Poor pay, work conditions drive nurses to UK hospitals
- Nigeria, Zimbabwe consider laws to tackle brain drain
LAGOS – Emem Isong screamed in pain on a trolley outside a hospital accident and emergency department in Nigeria's biggest city after a car ran over her foot and broke two of her toes.
"Please hold on ... there are just three of us on duty," a nurse at the Ebute-Metta federal medical centre in Lagos told the 33-year-old. "The alternative is for you to go to another hospital."
After a five-hour wait, nurses tended to Isong's wounds.
"It was either I wait till it is my turn or they refer me to another hospital that will turn me away," said Isong.
Nigeria, like many other African countries, is suffering a flight of talent from its fragile healthcare sector as richer countries woo underpaid but skilled professionals - a situation its government hopes to remedy with new legislation.
Michael Nnachi, president of Nigeria's nursing union, said more than 11,000 of 150,000 members had left the workforce since the COVID-19 pandemic to seek better pay and conditions abroad.
The economic downturn in Nigeria has only boosted the trend, said the nursing union's chairman, Olurotimi Awojide.
"Food, transport and rent are high, and money they pay now can't meet our needs. Nurses feel they need to go out of the country to live a better life," he said.
New to Context? We'd love for you to find out a little more about what we do. Click here for a selection of our best work.
Nigeria has been on the World Health Organization's (WHO) list of countries with a shortage of healthcare workers since 2020. Foreign employers are discouraged from recruiting nurses from the list, two-thirds of which this year are African states.
But the list has proven ineffective in stemming the exodus and Nigerian hospital managers say patient care is suffering as there are not enough new nurses to replace those moving abroad.
Wasiu Adeyemo has managed Lagos University Teaching Hospital for more than a decade, but said he has never seen staff shortages as bad as now.
Four wards with more than 90 beds remain shut at the facility, one of Nigeria's biggest specialist hospitals, with no nurses to operate them.
"Everyone talks about doctors leaving when the real problem we're facing is nurses going daily," Adeyemo told Context.
"At this point, are we saying we're going to hire nurses from Sudan or Cuba?" he asked. "Few nurses apply for jobs, and when we employ them ... about 50% will resign after three months to go to the UK."
Thousands of Nigerian nurses come to UK
Britain is the favoured destination for Nigerian nurses.
Last year, 7,200 Nigerian nurses were registered with the Nursing and Midwifery Council, Britain's professional body. Only the Philippines and India had more nurses in Britain.
The British government says employers should not actively recruit from places like Nigeria on what it calls the "red list" of countries where the WHO says there is a shortage of healthcare workers. But candidates from those countries can still apply for jobs advertised in Britain.
Nigerians received 12% of the skilled health and care worker visas issued last year, Britain's Home Office said.
Nigerian nurse Josephine is about to add to the number. The 28-year-old said she resigned from one of Nigeria's leading cancer care hospitals after receiving a UK visa last month.
Her husband sold their car and she is selling furniture and appliances before taking up her new job as a critical care nurse in the private sector in Britain.
The mother-of-two, who asked for her surname not to be used, said it was increasingly hard to live on her 100,000 naira ($135) monthly salary.
"I'm on duty at hospital all weekend, away from my children, all to be paid peanuts at the end of the month," Josephine said.
Her British employers will pay 20 times what she now earns, she said.
Skilled health worker visas
Although Zimbabwe is much smaller than Nigeria, it was the number one African country receiving skilled health workers' visas from the UK - accounting for 16% last year.
Before she came to Britain, Tendai earned about $200 a month as a senior nurse in Zimbabwe. The mother-of-three moved two years ago for a better career and better future for her children.
Her take-home pay at a hospital in the south of England is more than 10 times her salary back home. Though the high cost of living means half her salary goes on rent and bills, she does not have to pay for her daughters' schooling.
"Life in the UK is expensive, but at the end of the day, you are able to afford the basics. I know my kids have the basic things in terms of food, clothes ... compared to back home," said Tendai, who asked for her real name not to be used.
More than 4,000 doctors and nurses have left Zimbabwe since 2021, according to its Health Services Board.
Laws planned to stop exodus
Zimbabwe was added to the WHO list of countries where health workers should not be recruited for the first time in March.
Tendai said many nurses who had paid to take English-language tests and process travel documents were unhappy as it made getting jobs abroad harder without recruiters' help.
"Some nurses have lost a lot of money - because they had done all these things," she said. "People spend two years working towards coming to the UK and then, when you think you are almost there, the red list comes."
Zimbabwean Health Minister Constantino Chiwenga said plans were underway to criminalise the foreign recruitment of health professionals and retain the workforce, local media reported.
Back in Nigeria, lawmakers have passed a bill to withhold licences from doctors and dentists until they have practised in the country for five years. The president has yet to sign the bill into law, but one parliamentarian already wants to put the same restrictions on nurses and pharmacists.
Doctors have threatened strike action in response.
"It is a lazy approach," said Jesse Otegbayo, professor of medicine at the University College Hospital in the southwestern city of Ibadan. Instead, the government should address health workers' concerns, he said.
James Avoka Asamani, a WHO expert in Africa, said richer nations should compensate countries that had trained health workers to make the process mutually beneficial.
"If another country has used their public resources to train health workers, and you are recruiting them, it is only morally justified that you also invest in that health system to protect it from collapse," Asamani said.
But for now, Otegbayo said hospitals in Nigeria were on the brink, with many nurses complaining of burnout.
"This is a serious situation ... any health administrator and the public should be worried. The few nurses that are left are overworked, and this will affect the patients," he said.
(Reporting by Bukola Adebayo. Additional reporting by Emma Batha in London. Editing by Jon Hemming.)
Context is powered by the Thomson Reuters Foundation Newsroom.
Our Standards: Thomson Reuters Trust Principles
Tags
- Pay gaps
- Wealth inequality
- Cost of living
- Migration
- Future of work
- Workers' rights
- Economic inclusion